
Hallux Limitus
Hallux Limitus is a condition causing inflammation and soreness

Biomechanical Treatment for Moderate-to-Severe Hallux Abducto Valgus
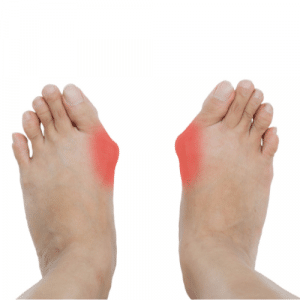
Recently we posted an article about various forefoot deformities. Here we focus on moderate to severe hallux abducto valgus, and look at treatment options. As stated in the previous blog,
once the deformity has progressed to the stage where bowstringing of the flexor hallucis longus and extensor hallucis longus have initiated an increase in the intermetatarsal angle, then orthotics alone will not control the deformity, and surgical correction and orthotics and/or digital orthoses are indicated.”
The moderate to severe bunion deformity is becoming an ever-increasing occurrence fur to our aging population. This article will show you the correct orthotic prescription to relieve symptoms and to stop further acquired deformity. Following these treatment options assumes that surgical intervention is not yet warranted or preferred.
A rearfoot varus is almost always present alongside the hallux abducto valgus deformity. On the orthotic, a rearfoot post of 4-5 degrees is most sensible when deciding the amount of rearfoot varus to use. After casting, check the amount of forefoot varus or valgus in the cast. If you see high degrees in either direction consider decreasing the rearfoot varus post.

Where we may see a lack of awareness in treating this deformity is the malposition of the first metatarsal. The first metatarsal is usually deviated medially from the second metatarsal and it is hyper mobile. Also, the first metatarsal is often short in relation to the second metatarsal. This can be due to a basic anatomical deformity as seen in the Morton’s type foot. But oftentimes, the first metatarsal becomes short as the entire shaft drifts medially as the deformity progresses. The proper orthotic posting to order is a first metatarsal cut out. If there is little mobility of the first metatarsal then just a cut out is sufficient. However, some of these deformities require a 1/8″ bar along with a first metatarsal cut out, which is essentially a 1/8″ raise from the second metatarsal to the fifth. This will effectively transfer more weight onto the first metatarsal. In this deformity, little if any weight is bearing on the first metatarsal which promotes medial deviation of the first metatarsal and lateral deviation of the hallux.
The next step is to choose an orthotic device that will apply these postings correctly but not significantly decrease space in the patient’s shoe. A low bulk device is best. The practitioner may choose not to include any extensions or excess padding in order to decrease bulk as much as necessary.
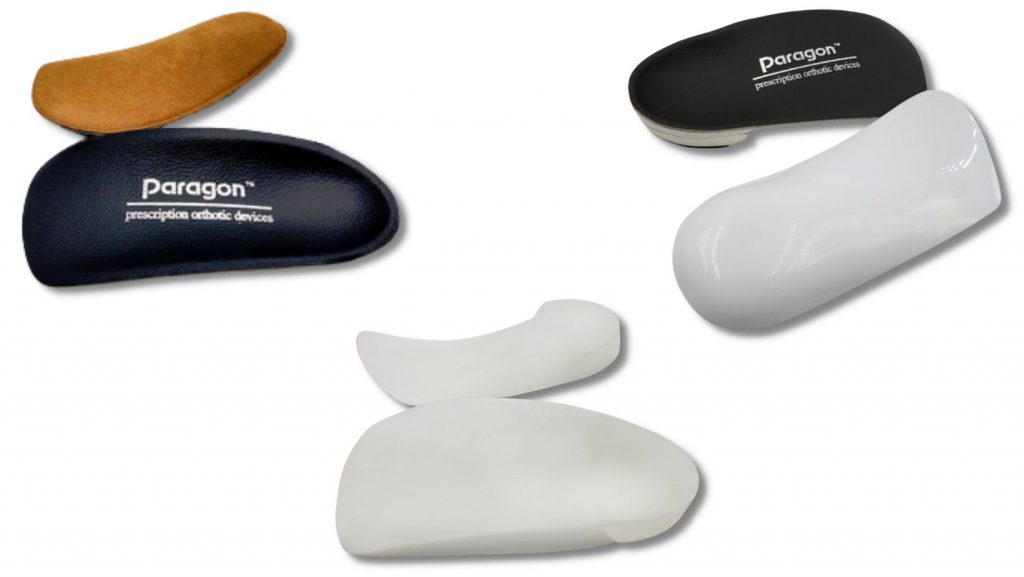
At this point, we recommend the patient have a two week trial period wearing the orthotics. Any adjustments should be made prior to the next and very important treatment step- the digital orthoses.
The acquired forefoot deformity associated with hallux abducto valgus may be the most overlooked and undertreated problem in podiatry. It will not stop progressing in severity with orthotics alone. A digital orthosis is needed to prevent further acquired deformity and increase dorsiflexion of the forefoot. Use of digital orthoses will effectively increase the stride length, benefiting the hip and lower back. Also, by filling available space between the toes, the progression of deformity is reduced dramatically.
Patient management should include informing the patient on the first visit that wearing these digital appliances will be necessary to stop further progression of the deformity. The patient should also be made aware that fabrication of these appliances might require multiple visits.
After you have conducted a one to two week trial with the orthotics, made any required adjustments and determined that the orthotics are correctly posted, then fabrication of the digital orthoses can commence.
Start with the fabrication of a device for the most symptomatic foot. Never do both feet at the same time. A trial period is needed to determine patient acceptance. Although the device may be comfortable in the office/clinic, it may become intolerable after a short walk. The patient should know from the outset that the trial and error method is used to obtain the correct fit.

The initial step is to choose the correct amount of compound. Make sure to use vinyl gloves when handling the compound. Use the minimal amount of compound to fill the available space; most problems occur from using too much compound. Also, the amount of catalyst needed to make a typical device is usually less than the manufacturer recommends. A jar of D.O.C. (Digital Orthosis Compound) comes with two tubes of hardener paste, which is much more than needed to catalyze the whole jar. More catalyst will create a harder device and have a quicker setting time; it will take practice, and experience, to learn how much to use.
The space I usually try to fill is from the 1st interspace to the 3rd interspace. However, the variation of shapes is different from patient to patient.
The next step is to add the hardener (photo 1). Repeatedly fold the compound over the hardener until it is a uniform colour. Place the compound in the sulcus and press gently into place while holding the forefoot, as if the foot was bearing weight. At this point slip a knee-high stocking over the foot (photo 2). Replace the patient’s shoe with the orthotic in place and have the patient bear weight (standing for about one minute). Remove the shoe and stocking and examine the device. (photo 2) Sometimes excess compound will need to be trimmed with scissors. After the device is fully cured, it may need to be shaped with a grinder.


Be prepared to repeat the fabrication process until the correct shape is achieved. Don’t give up. This device is an indispensable treatment tool, especially useful for treating hallux abducto valgus.
I usually have the patient return after wearing the device for one week. If the patient is satisfied with it, I proceed to fabricate a device for the opposite foot. Always insist on the device for both feet. An uneven stride length can cause hip and back pain.
Although this treatment is relatively simple, do not underrate it. Your patient needs to feel that it is valuable enough to go through with the treatment and comply with wearing the device on a daily basis.
After the final device has been made, let the patient know that due to straightening of the lesser toes a new device may be needed in about one year’s time. If the casting procedure has been done correctly, the lesser toes may begin to de-contract and straightening will indeed occur. If the device is not replaced, its effectiveness decreases and the deformity will begin to worsen once again.
It takes time, effort, and patience to develop the skills required to use this material correctly. If you put in the work, you will be amazed at the superior results you will obtain.


Hallux Limitus is a condition causing inflammation and soreness

Patient Female, 62 years old, 165 lbs. Complaints Pain at

When considering older patients in any context it’s best to
| Cookie | Duration | Description |
|---|---|---|
| cookielawinfo-checkbox-analytics | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookie is used to store the user consent for the cookies in the category "Analytics". |
| cookielawinfo-checkbox-functional | 11 months | The cookie is set by GDPR cookie consent to record the user consent for the cookies in the category "Functional". |
| cookielawinfo-checkbox-necessary | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookies is used to store the user consent for the cookies in the category "Necessary". |
| cookielawinfo-checkbox-others | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookie is used to store the user consent for the cookies in the category "Other. |
| cookielawinfo-checkbox-performance | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookie is used to store the user consent for the cookies in the category "Performance". |
| viewed_cookie_policy | 11 months | The cookie is set by the GDPR Cookie Consent plugin and is used to store whether or not user has consented to the use of cookies. It does not store any personal data. |