
Patient Centered Care
The concept of patient centered care may sound pretty basic,


Shin splints are a painful injury, common among athletes, soldiers and dancers. They are one of a number of injuries caused by repetitive overuse of leg muscles. Many of those who have sustained injury are unaware of the causes and proper treatment.
There are two ways to look at shin splints: clinically and practically. First, let’s examine the medical basics.
The lower leg is composed of two bones. The tibia (shin bone) and the fibula extend from ankle to the knee. There are eleven muscles in the leg, originating from one of both of those bones. The muscles are encased in four fibrous compartments. Within these compartments runs a neurovascular bundle comprised of nerves and blood vessels. Consequently, muscle movement during exercise is performed in a tight, enclosed space and is bound by a fairly inelastic fibrous retaining wall.
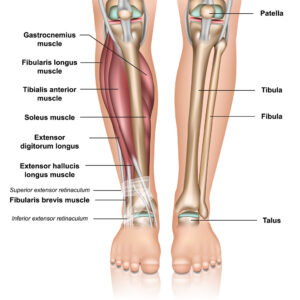
There is an elevation of compartment pressure in the leg after exercise. What exactly produces this increased pressure is a matter of speculation. One probable cause is the limit of compartment size, a result of the thickened fascial covering. Another probable cause is the volume within the compartment, a result of enlarged muscle hemorrhage from torn muscle fibers. Prolonged exercise can produce an increase in muscle bulk up to 20%.
The American Medical Association defines shin splints as “an inflammation of muscles that lead from the shin to the foot resulting from unaccustomed repetitive activity or forcible use of foot flexors”. The term “shin splints” is used to describe lower leg pain brought on by athletics. This pain includes any combination or all of the following: inflammation of the bone covering (periostitis), muscle inflammation (myostitis), and tendon inflammation (tendonitits). Despite the gloomy sounds of this physiological stat, shin splint victims can take comfort in one thing. Lower leg pain of this type rarely requires surgery.
The two most common types of shin splints are Posterior Tibial and Anterior Tibial. With the former, pain extends along the inside or medial back of the lower leg and ankle. With the latter, pain is centered in the lower front of the shin and down the outside or lateral border. Three factors contribute to the overuse of the lower leg muscles: muscle imbalance, running on hard surfaces, and pronated feet.

The basic treatment for shin splints is RICE – rest, ice, compression, and elevation, accompanied by the appropriate amount of over-the-counter pain relievers to help to lessen pain and inflammation. By the third recovery day begin alternating ice therapy and foot exercises. Deep friction massages before bedtime are also beneficial.
Orthotic therapy can properly align the foot during gait and correct any muscle imbalances that may have been a contributing source of the problem. As well, supporting the arches will reduce any foot pain that has accompanied the shin inflammation. A heel lift reduce strain on overworked lower leg muscles, used in both shoes. Practical recovery from shin splints requires common sense.
Initiating a flexibility and strengthening program for lower legs is an excellent preventative measure. Special attention should be paid to the Achilles tendon, the calf and the tibial muscles, both anterior and posterior. Other ways to prevent shin splints or lessen the pain include running on softer surfaces and using shock absorbing yet flexible shoes. Wearing foot orthotics works as a preventative measure in order to correct two of the factors contributing to lower leg overuse; muscle imbalance and pronated feet. Paragon offers a variety of device types and styles that can be used as a preventative and/or treatment option for shin splints.


The concept of patient centered care may sound pretty basic,
Communicating the Etiology of Diabetic Foot Ulcers to Patients Gustav

Hallux Limitus is a condition causing inflammation and soreness
| Cookie | Duration | Description |
|---|---|---|
| cookielawinfo-checkbox-analytics | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookie is used to store the user consent for the cookies in the category "Analytics". |
| cookielawinfo-checkbox-functional | 11 months | The cookie is set by GDPR cookie consent to record the user consent for the cookies in the category "Functional". |
| cookielawinfo-checkbox-necessary | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookies is used to store the user consent for the cookies in the category "Necessary". |
| cookielawinfo-checkbox-others | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookie is used to store the user consent for the cookies in the category "Other. |
| cookielawinfo-checkbox-performance | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookie is used to store the user consent for the cookies in the category "Performance". |
| viewed_cookie_policy | 11 months | The cookie is set by the GDPR Cookie Consent plugin and is used to store whether or not user has consented to the use of cookies. It does not store any personal data. |